QUICK LINKS: Practice Support Tools | Patients | Find a Neuro-Ophthalmologist | NOVEL | YONO Portal | Our Journal | Fellowships
Droopy Eyelids (ptosis)
Patients: Download as PDF
Clinicians: Download as PDF
What is a droopy eyelid (ptosis)?
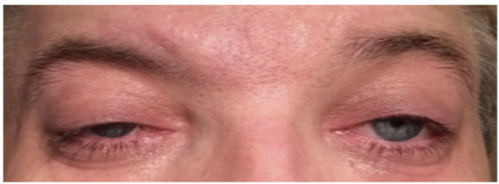
Eyelid ptosis is the medical term used to describe a droopy upper eyelid. Eyelid ptosis occurs naturally as we age, but some medical emergencies and diseases can cause eyelid ptosis too. Eyelid ptosis can affect one or both eyes. Sudden onset of eyelid ptosis is a medical emergency.
 |
What additional symptoms are worrisome?
If you experience sudden headache, neck pain, facial droop, eye pain, blurry vision, double vision, changes in pupil size, vertigo, difficulty speaking and/or difficulty swallowing, immediately call 911 or seek care in an emergency room.
What causes a droopy eyelid (ptosis)?
As we age, gravity causes the eyelids to become more droopy. Age-related eyelid ptosis typically affects both upper eyelids somewhat symmetrically. The frequent eyelid manipulation required to insert and remove contact lenses can stretch the eyelid muscles over time, causing eyelid ptosis. Similarly, when an eyelid is held open during surgery, like cataract surgery, the eyelid muscles can stretch and the eyelid can become droopy. Chronic use of steroid eye drops can also produce stretch of the eyelid tissues over time, resulting in ptosis. Some children are born with droopy eyelids. This congenital ptosis must be monitored closely. If the droopy eyelid interferes with visual development, the child may need timely surgery.
However, all of these more benign causes of eyelid droop do not cause complete ptosis (complete eyelid closure), which should be considered a sign of a potential neurological problem. Sometimes a droopy eyelid may indicate a serious problem inside the brain, neck, or eye socket. Sudden onset of eyelid ptosis could be a sign of a stroke, aneurysm, or tear in the carotid artery in the neck. You should go to an emergency room immediately if you suddenly develop a droopy eyelid, with or without associated pain around the eye or face.
Eyelid ptosis can also be a symptom of underlying systemic autoimmune disease or even cancer. Ocular myasthenia gravis (OMG) is an autoimmune condition that frequently causes eyelid ptosis and double vision. Thyroid eye disease (TED) can cause eyelid retraction, which means that the lid is pulled up higher than normal, which can give the illusion of eyelid ptosis on the opposite side in some patients. Some chronic muscle disorders can manifest first with ptosis.
Eyelid ptosis can result from excess fluid retention, allergies, or infections that cause eyelid swelling. An eyelid growth or vascular malformation can also cause the eyelid to droop.
Why do I need to see a neuro-ophthalmologist?
Neuro-ophthalmologists have expertise that can help determine the cause of eyelid ptosis, whether any additional testing is needed, and if there are potential medical or surgical treatments.
How do you treat eyelid ptosis?
The treatment of eyelid ptosis depends on the cause. For example, if eyelid ptosis is caused by myasthenia gravis, daily oral medication is the first treatment. A droopy eyelid caused by a stroke may improve over time as the body heals. Some droopy eyelids even improve with prescription eye drops.
Many patients require surgical eyelid ptosis repair. Neuro-ophthalmologists often perform eyelid ptosis surgery, but some may refer you to an oculoplastic surgeon. Surgery is performed in an operating room but typically does not require an overnight hospital stay. Over time, the eyelid can droop again, potentially requiring multiple surgeries in a lifetime.
If eyelid ptosis is severe enough to interfere with normal vision, surgery is often covered by insurance. Surgical repair of mild eyelid ptosis may be considered cosmetic surgery. Each insurance plan is unique. Your surgeon will help you determine your specific coverage.
Additional Reading/Resources
Other Websites
- American Academy of Ophthalmology Eyewiki: https://eyewiki.org/Blepharoptosis
- American Academy of Ophthalmology Eyewiki: https://eyewiki.org/Myogenic_Ptosis
- American Academy of Ophthalmology Eyewiki: https://eyewiki.org/Myasthenia_Gravis
- American Society of Ophthalmic and Reconstructive surgery: https://www.asoprs.org/droopy-eyelids--ptosis-
Copyright © 2024. North American Neuro-Ophthalmology Society. All rights reserved.
This information was developed collaboratively by the Patient Information Committee of the North American Neuro-Ophthalmology Society. This has been written by neuro-ophthalmologists and has been edited, updated, and peer-reviewed by multiple neuro-ophthalmologists. The views expressed in this brochure are of the contributors and not their employers or other organizations. Please note we have made every effort to ensure the content of this is correct at time of publication, but remember that information about the condition and drugs may change. Major revisions are performed on a periodic basis.
This information is produced and made available “as is” without warranty and for informational and educational purposes only and do not constitute, and should not be used as a substitute for, medical advice, diagnosis, or treatment. Patients and other members of the general public should always seek the advice of a physician or other qualified healthcare professional regarding personal health or medical conditions.