QUICK LINKS: Practice Support Tools | Patients | Find a Neuro-Ophthalmologist | NOVEL | YONO Portal | Our Journal | Fellowships
Anisocoria
Patients: Download as PDF
Clinicians: Download as PDF
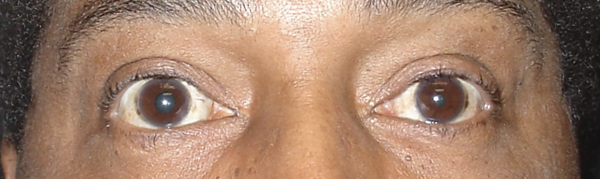
Courtesy of Scott Haines, M.D.
What is anisocoria?
Anisocoria is a medical term for unequal pupil size. Normally our pupils are relatively the same size. While small differences in pupil size are normal and can even come and go (physiologic anisocoria), constant and significant differences in pupil sizes may be a sign of damage to the brain or the nerves that control the pupils.
What causes anisocoria?
Normally, in dim light (such as at night), the pupil dilates (becomes larger) to let in more light to the eyes. In bright light (such as sunlight), the pupil constricts (becomes smaller), which decreases the amount of light getting into the eye. Problems affecting the muscles or nerves controlling the pupil cause abnormal pupil size. When this affects one side, the pupil sizes may be unequal.
Why should I be concerned about anisocoria?
Anisocoria cannot make you go blind. Though many causes of anisocoria are benign and some people only notice some blurry vision and/or light sensitivity, it can be a sign of a serious and potentially life-threatening neurological problem.
Horner Syndrome: An Abnormally Small Pupil
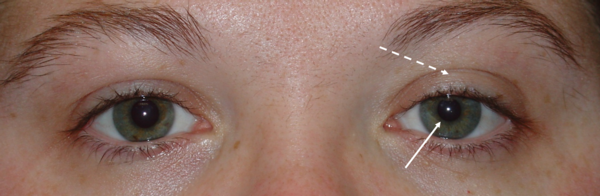
Courtesy of Scott Haines, M.D.
Left Horner syndrome. The left pupil is smaller (solid arrow) and the left eyelid is droopy (dashed arrow).
The nerves controlling the muscles that dilate the pupil are part of the sympathetic (“fight or flight”) nervous system. These nerves also control the muscles that open your eyelids and activate the sweat glands on your face. Horner syndrome occurs when these nerves do not work. The pupil on the affected side is abnormally small (miosis) and the upper eyelid will droop (ptosis) mildly. There also may be loss of sweating, especially on the forehead on the same side.
Horner syndrome does not damage the eye or cause vision loss. Although there are benign causes that do not usually need treatment, it is important to find out what is causing the Horner syndrome because it may be a sign of a life-threatening condition, such as stroke, lung, chest or brain tumor, or break in the wall of the carotid artery (carotid dissection). Experiencing pain in the neck or around the eye, in association with a Horner syndrome, may be a sign of a carotid dissection, and warrants urgent evaluation through the emergency department, since a dissection can lead to a stroke.
3rd Cranial Nerve Palsy: An Abnormally Large Pupil
The nerves controlling the muscles that constrict the pupil are part of the parasympathetic nervous system. These nerves travel along the 3rd cranial nerve, which comes from the brainstem near the back of your brain and travels forward to your eye. The 3rd cranial nerve also controls the muscles that move your eyes up, down, and in, as well as open your eyelid. Damage to the 3rd cranial nerve can result in a dilated pupil, droopy eyelid and double vision (when the lid is lifted) because the eye does not move normally. The affected eye can often appear deviated toward the ear and slightly downward. The pupil may or may not be dilated, but if it is, it requires urgent evaluation.
.png)
Courtesy of Valerie Biousse, M.D.
Right 3rd cranial nerve palsy. The right pupil is bigger (arrow) and the right eye is positioned down and out. A finger is holding the right eyelid open because it is so droopy.
The most concerning cause of a 3rd cranial nerve palsy is a brain aneurysm. This is a life-threatening medical emergency because the aneurysm can break open and bleed into the brain. Other causes of 3rd cranial nerve palsy include decreased blood flow to the nerve (microvascular ischemia), tumors pressing on the nerve, and inflammation of the nerve. Although these problems can be serious, they may improve with treatment (inflammation), without treatment (microvascular ischemia), or slowly worsen over time (tumor).
Are there other forms of anisocoria that are not dangerous?
Adie Tonic Pupil: An Abnormally Large Pupil
An Adie tonic pupil is abnormally large like a 3rd cranial nerve palsy, but the pupil still constricts when focusing on something close to the face, and there is no double vision or droopy eyelid. The eyes can move fully in all directions. It may occur after a viral infection, but usually no known cause is found. The pupil may remain large or gradually shrink in size over several years. Patients can note increased light sensitivity and blurriness when reading, but overall no specific treatment is needed. Your doctor may also find decreased reflexes in your legs but leg weakness does not occur.
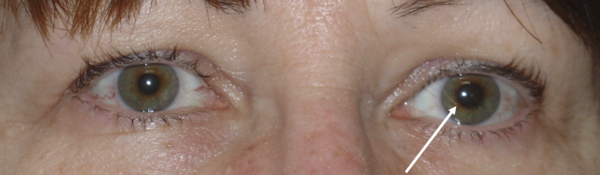
Left Adie tonic pupil. The left pupil is larger (arrow) and does not react to light.
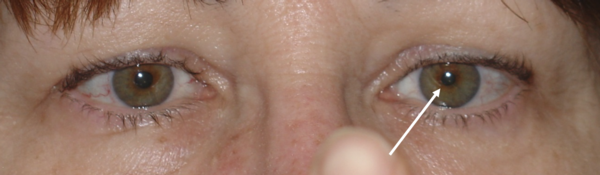
Left Adie tonic pupil. When focusing on the finger up close, the left pupil constricts more strongly (arrow).
Courtesy of Scott Haines, M.D.
Medications Or Chemicals Causing Anisocoria
There are many medications or chemicals that can cause the pupil to dilate or constrict. While some of these medications are intentionally used in the eye, sometimes these medications or chemicals are accidentally rubbed into the eye from your skin, usually by your finger.
- Eye drops that dilate the pupil: atropine, phenylephrine, tropicamide, cyclopentolate, scopolamine
- Eye drops that constrict the pupil: pilocarpine, brimonidine
- Other chemicals that affect the pupils: pesticides, the ingredients on flea collars, scopolamine skin patches for motion sickness, inhalers for asthma, antiperspirant wipes
A pupil that is chemically dilated or constricted will return to normal size and function as the chemical wears off. Depending on the specific chemical, this can take hours or days.
Why do I need to see a neuro-ophthalmologist?
Neuro-ophthalmologists specialize in conditions that cause problems with the pupils. Your doctor will examine your pupils in different lighting conditions and perform an eye and cranial nerve exam. Because some forms of anisocoria may be present for years before it is noticed, your doctor may ask you to provide old pictures to determine how long you have had the problem. Eye drops may be used to help diagnose the cause of the anisocoria. Your doctor may order scans of your head and body, such as MRIs and/or CTs. If these tests find any serious problems, your doctor will refer you to the appropriate specialists for urgent treatment. In other cases, they may recommend treatments for your symptoms, which could involve eye drops or nothing at all.
Additional Reading/Resources
- Anisocoria, by the American Academy of Ophthalmology’s EyeWiki Project (http://eyewiki.org/Anisocoria)
- Anisocoria, by Medlineplus (http://medlineplus.gov/ency/article/003314.htm)
- Anisocoria, University of Florida Health (https://ufhealth.org/anisocoria)
Copyright © 2023. North American Neuro-Ophthalmology Society. All rights reserved.
This information was developed collaboratively by the Patient Information Committee of the North American Neuro-Ophthalmology Society. This has been written by neuro-ophthalmologists and has been edited, updated, and peer-reviewed by multiple neuro-ophthalmologists. The views expressed in this brochure are of the contributors and not their employers or other organizations. Please note we have made every effort to ensure the content of this is correct at time of publication, but remember that information about the condition and drugs may change. Major revisions are performed on a periodic basis.
This information is produced and made available “as is” without warranty and for informational and educational purposes only and do not constitute, and should not be used as a substitute for, medical advice, diagnosis, or treatment. Patients and other members of the general public should always seek the advice of a physician or other qualified healthcare professional regarding personal health or medical conditions.