QUICK LINKS: Practice Support Tools | Patients | Find a Neuro-Ophthalmologist | NOVEL | YONO Portal | Our Journal | Fellowships
Transient Vision Loss
Patients: Download as PDF
Clinicians: Download as PDF
What is transient visual loss?
Transient visual loss is the term used to describe loss of part or all of the vision in one or both eyes temporarily. Some people do not experience a complete loss of the affected vision and instead describe the abnormality as “blurring” or like “looking through a veil.” The vision typically returns to normal before a person is able to be examined by an ophthalmologist, so the examination may be normal. Undergoing an eye examination is still very important, as diagnostic clues can sometimes help an eye doctor narrow down the possible causes. Even if the vision returns to normal, transient visual loss can be a sign of serious abnormalities of the eye, brain, or blood vessels that can lead to permanent vision loss or even to a brain stroke, without prompt recognition and treatment.
Why is it important to be evaluated quickly after an episode of transient visual loss?
If the vision loss episode is thought to be due to a blood clot blocking the flow of blood to a part of your eye or brain, this is treated in the same way as a transient ischemic attack (TIA; temporary blood flow interruption in the brain) or stroke. Urgent evaluation in an emergency department that can treat patients for stroke is necessary. There, health care providers can evaluate the patient, and if a blood clot is suspected to be the cause of transient visual loss, further testing may be performed. Evaluations may include an MRI of the brain, blood vessel imaging of the head and neck, bloodwork including your cholesterol levels, heart rhythm monitoring (electrocardiogram), and an ultrasound of the heart (echocardiogram). The results of these tests will help determine the best treatments to help protect your vision and brain from future damage. Medicines that reduce blood clotting such as aspirin may be started, and in some cases, a surgery to open up blockage in a neck artery or placement of a stent in the artery, may be recommended.
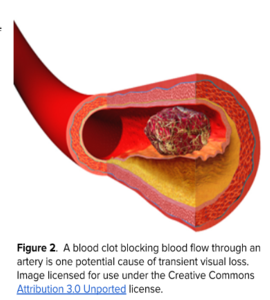
What if my transient visual loss is not related to a blood clot?
Other causes of transient visual loss can still be serious or may be benign. Based on your description of your visual loss events and the help of other tests, your health care provider can provide more details about the specific cause of your visual loss episodes.
What are some causes of transient visual loss that may only affect one eye?
- Blood clot from the arteries or heart
- Blood vessel inflammation (vasculitis, such as giant cell arteritis)
- Blood vessel malformation or tumor in the eye socket (orbit)
- Spasm of blood vessels feeding the eye (retinal vasospasm)
- Optic nerve swelling
- Angle-closure glaucoma
- Dry eyes
- Spasm of muscle that focuses the lens inside the eye
What are some causes of transient visual loss that affect both eyes simultaneously and to the same degree?
- Migraine (common, and can occur even without headache)
- Transient ischemic attack (temporary interruption of blood flow to the back part of the brain – occipital lobes)
- Seizure (involving the back part of the brain – occipital lobes)
- Swelling of both optic nerves (papilledema, related to high pressure in the brain)
- Presyncope (temporarily decreased blood flow to the brain that can cause lightheadedness and decreased vision)
- Changes in blood glucose level, especially in diabetics
What details of my vision loss episodes are important to keep track of?
As your eye examination may be normal after an episode of transient visual loss, the details of your episodes are very important in determining the cause and what to do next. Keeping careful track of the answers to the following questions can help narrow down the possibilities:

- Did the vision loss involve one or both eyes?
- Did you try closing each eye to check?
- If it involved both eyes, was it simultaneous and exactly the same in the two eyes?
- How long did the vision loss last (seconds, minutes, hours)?
- What part of the vision was affected? For example, was it the left or right side, top or bottom?
- Could you see through the area of vision loss or was the missing area completely dark? Or like a “white out?”
- Did you see anything that wasn’t really there, like shapes, colors, or lights?
- How did the vision loss start? Did it come on gradually or suddenly?
- Over what period of time did the vision improve? Gradually or suddenly back to normal?
- How many episodes of vision loss have you had?
- If the vision loss episodes involved one eye or one side, did the vision loss ever happen on the other side or in the other eye?
- Did you have any other symptoms during or right after your episodes of vision loss? For example, was there a headache, light or sound sensitivity, dizziness, eye discomfort or other neurologic symptoms?
- Can you think of any factors or activities that trigger the vision loss episodes?
- Once the vision loss occurs, is there anything you can do to bring the vision back more quickly?
What details of my medical history are important to share with my healthcare provider evaluating me for transient visual loss?
- Any history of conditions that affect blood vessels such as diabetes, high cholesterol, high blood pressure, smoking, sleep apnea, or abnormal blood clots.
- Any history of stroke, heart attack, heart rhythm problems, or blood vessel narrowing in the neck (carotid stenosis)
- Any eye conditions, such as glaucoma or past vision loss episodes
- Temporary episodes of neurologic symptoms in the past
- If over age 50, any history of headaches, scalp tenderness, jaw pain with chewing, fevers, unexplained weight loss, a new change in energy level, double vision, loss of appetite, stiffness/pain in shoulders/hips
- A history of migraine
What is amaurosis fugax?
Amaurosis fugax is a mix of terms from Greek (amauros – “dark”) and Latin (fugax – “fleeting”) that refers to a temporary loss of vision in one eye from an interruption in blood flow. This term is not typically used to describe other forms of transient visual loss.
Additional Reading/Resources
Other Websites
- Transient Ischemic Attack Overview, by UpToDate® (https://www.uptodate.com/contents/transient-ischemic-attack-beyond-the-basics#)
- Migraine with aura, from the Mayo Clinic (https://www.mayoclinic.org/diseases-conditions/migraine-with-aura/symptoms-causes/syc-20352072)
Copyright © 2023. North American Neuro-Ophthalmology Society. All rights reserved.
This information was developed collaboratively by the Patient Information Committee of the North American Neuro-Ophthalmology Society. This has been written by neuro-ophthalmologists and has been edited, updated, and peer-reviewed by multiple neuro-ophthalmologists. The views expressed in this brochure are of the contributors and not their employers or other organizations. Please note we have made every effort to ensure the content of this is correct at time of publication, but remember that information about the condition and drugs may change. Major revisions are performed on a periodic basis.
This information is produced and made available “as is” without warranty and for informational and educational purposes only and do not constitute, and should not be used as a substitute for, medical advice, diagnosis, or treatment. Patients and other members of the general public should always seek the advice of a physician or other qualified healthcare professional regarding personal health or medical conditions.











_200x72(2).png)